Capabilities & outcomes
What organisations should expect when imaging workflow software is engineered for Australian healthcare constraints: throughput, safety, interoperability, and accountability—not a list of features divorced from delivery.
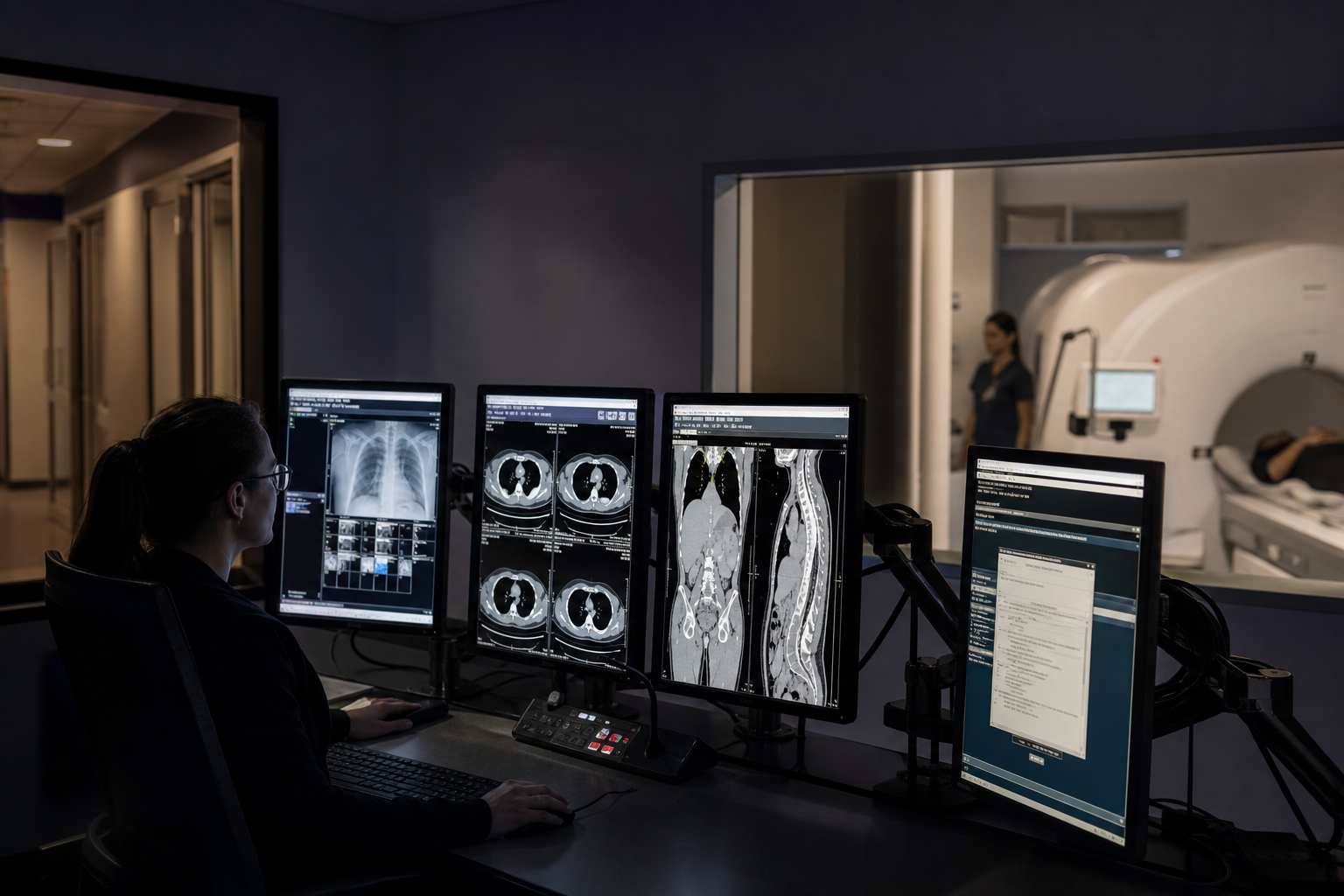
Capabilities only matter if they translate into measurable outcomes: fewer manual reconciliations, faster turnaround without corner-cutting, and reporting consistency that survives peer review and external audit.
The programmes that succeed treat adoption as part of the specification. Training, change management, and operational telemetry are not “phase two”—they are how you prove the system works in February, not only on go-live day.
Turnaround and safety under real roster conditions
Capability statements mean little without time-based measures stratified by priority class: ED, inpatient, outpatient cancer pathways, and routine elective work each carry different risk profiles. We encourage customers to define acceptance tests in those lanes—not only aggregate “median report time” charts that hide tail risk.
Safety-related capabilities include addendum discipline, peer-learning workflow support, and tooling that reduces wrong-patient/wrong-study selection through ergonomics and logging—not only through training posters.
Interoperability outcomes, not interface counts
“Connected” should mean reconciled: orders map to encounters, reports land in the correct chart tab, and failures are visible before they become patient-visible delays. Capability discussions should include reconciliation logic, monitoring, and ownership when vendors disagree about semantics.
Governance: templates, privileges, and evidence
Outcomes depend on controls: who can publish template changes, how break-glass access is granted, and whether your audit exports can answer medico-legal questions without a multi-week forensics project. Those governance capabilities are as important as any new image-processing feature.